Group and family therapy sessions involve multiple people sharing sensitive information in a single room. This creates unique legal and ethical challenges that therapists must navigate carefully.
We at Billie Jo Hopwood Family Law & Mediation, PLLC understand that the legal and ethical considerations for group and family therapy extend far beyond standard one-on-one practice. Confidentiality rules shift when multiple participants are present, consent becomes more complex, and reporting obligations can create difficult situations.
Confidentiality and Privacy in Group and Family Therapy
When multiple people sit in the same room discussing personal matters, confidentiality becomes complicated in ways that therapists often underestimate. The American Association for Marriage and Family Therapists revised its Code of Ethics on January 1, 2026, and made clear that therapists cannot guarantee confidentiality among group participants themselves-only within the therapist-client relationship. This distinction matters enormously. In individual therapy, you control who hears what. In group or family settings, you cannot control what participants tell others after they leave.
Establishing Confidentiality Norms Across Multiple Participants
The AAMFT standards require you to establish explicit group confidentiality norms and remind members regularly that while you maintain confidentiality, other participants may not. Your written informed consent documents must address this directly. Specify what information can be shared outside sessions, what remains private, and what happens if someone breaches group confidentiality. Many therapists skip this step or bury it in generic consent forms, then face complaints when a family member repeats something shared in a joint session. The APA Ethics Code and AAMFT guidance both insist on plain-language disclosure at the outset and ongoing reminders throughout treatment.

Your records must reflect these conversations. Document when you reviewed confidentiality limits, what you said, and how participants responded.
Managing Disclosures Between Family Members
In family therapy, managing disclosures between members creates constant ethical tension. One parent might tell you something about the other parent or about a child’s behavior that directly affects treatment. The revised AAMFT Code prohibits you from disclosing any individual’s confidences to others in the client unit without prior written permission from that individual. This applies even when full family sessions are happening. If a teenager reveals substance use in a private moment before a family session, you cannot tell the parents without the teen’s consent-unless safety is at stake. When safety concerns emerge, you must know your jurisdiction’s mandatory reporting laws. The duty to warn applies when imminent danger exists, but the threshold varies by location. Document your safety assessment, the specific danger you identified, and steps you took in response. A documented safety plan with emergency contacts and local crisis resources like the 988 Suicide & Crisis Lifeline protects both clients and your practice. Your records should show the clinical reasoning behind each decision to disclose or withhold information.
Record Retention and Access Requirements
The Medical Council of India guidelines recommend keeping records for at least three years, and many states require longer retention. When someone requests access to group or family therapy records, written authorization from each individual competent to consent is required-this means you cannot hand over records to one family member without permission from others, even if they all attended the same sessions. Physical and digital records must be stored separately from personal clinician notes and kept secure with limited access to authorized personnel. HIPAA compliance is non-negotiable for any practice handling protected health information, and many state licensing boards impose additional requirements beyond federal standards. When clients request their records, you have a short window to respond. The Medical Council of India requires responses within 72 hours, and many U.S. jurisdictions follow similar timelines.
Planning for Practice Changes and Data Security
Plan ahead for what happens to records if your practice closes, relocates, or changes ownership. Arrange secure storage, transfer, or disposal in compliance with your state’s laws. Breaches must be reported promptly to affected individuals and, depending on jurisdiction, to regulatory bodies. The cost of a breach notification far exceeds the cost of proper record management from day one. These confidentiality safeguards form the foundation for the next critical area: obtaining informed consent that actually protects both you and your clients.
Informed Consent and Ethical Boundaries
Informed consent in group and family therapy fails most therapists because they treat it as a checkbox rather than an ongoing conversation. The revised AAMFT Code of Ethics requires consent before starting services and throughout treatment, but many practitioners hand clients a generic form, get a signature, and never address consent again. This approach leaves you exposed legally and ethically.
Written Consent Documents That Protect Both Parties
Your written consent document must be understandable to the people who sign it-plain language matters more than legal precision here. Cover the specific risks and benefits of group or family treatment, not vague platitudes. State exactly what happens during sessions, how long they last, what the cancellation policy is, what fees apply, and what emergency procedures exist. Address technology use explicitly if you conduct telehealth sessions, including platform privacy limitations and cross-state licensure considerations. Most critically, explain that the therapist maintains confidentiality but other participants may not, and describe what happens if someone breaches confidentiality.

Consent as an Ongoing Process, Not a One-Time Event
The APA Ethics Code and ACA guidelines both emphasize that informed consent is not a one-time form but an evolving process. You should revisit key points periodically, especially before major treatment shifts or when new participants join. Document these conversations in your clinical notes. One therapist’s mistake was obtaining written consent for a couple’s therapy session, then later adding the couple’s adult child to sessions without updating the consent document or discussing how this changed confidentiality dynamics. That oversight created liability when the child later complained they weren’t informed about what information might be shared. Your consent document should specify how many people will participate, their roles, and what happens if the composition changes.
Identifying and Addressing Power Imbalances
Power imbalances in family and group settings require active intervention, not passive observation. The AAMFT Code prohibits abusing the therapeutic relationship for power and requires you to respect client autonomy. In family therapy, one parent often holds more financial or social power than the other, or a teenager may fear speaking openly because they live with the more dominant parent. In group settings, an older member or someone with higher status may inadvertently silence others. You must identify these imbalances early and address them directly in sessions.
Some therapists avoid this because it feels confrontational, but failing to address power dynamics violates your ethical duty. Establish explicit ground rules at the first session: everyone receives uninterrupted speaking time, no one can speak for another person, and interruptions are off-limits. In family therapy, consider individual sessions with each member before joint sessions begin. These private meetings let you understand each person’s perspective and safety concerns without others present.
Documenting Boundary Work and Interventions
The 2026 AAMFT Code requires clear boundaries within the therapeutic relationship, and part of that means preventing dominant participants from controlling the narrative. If one family member repeatedly interrupts or dismisses another, stop the session and address it. Say something like: “We’re going to pause here because I notice that pattern is happening again, and it prevents us from hearing everyone’s perspective.” If group members begin forming alliances that exclude or demean others, intervene immediately. Document these interventions in your progress notes because they demonstrate you recognized the power dynamic and took clinical action. Avoiding this documentation suggests you missed the problem entirely.
These boundary protections form the foundation for your legal obligations. Understanding when you must disclose information-and when you cannot-determines whether your practice survives scrutiny.
Mandatory Reporting and Legal Obligations
Mandatory reporting laws override confidentiality, and this reality creates the hardest decisions therapists face in group and family settings. The 2026 AAMFT Code of Ethics requires you to comply with laws regarding reporting of alleged unethical conduct, and state mandatory reporting statutes trump your ethical duty to keep information private. Most states require reports of child abuse and neglect, elder abuse, and imminent danger to self or others, but the specific triggers and timelines vary significantly by jurisdiction.
Know Your State’s Exact Reporting Requirements
Florida’s mandatory reporting law requires reports to the Department of Children and Families within 24 hours of learning about suspected child abuse or neglect, and failure to report is a felony if the person knew or should have known about the abuse. You cannot wait for a family session to end or consult with a supervisor before making that call. The moment you have reasonable suspicion, you must report. This means you need to know your state’s exact definitions before you ever see a family or group client.
Many therapists operate under vague assumptions about what counts as reportable abuse, then face licensing board complaints when they either over-report minor parenting disagreements or under-report actual harm. Get your state’s mandatory reporting statute in writing, highlight the specific triggering language, and keep it accessible during sessions. When a parent mentions spanking a child with a belt, you must know whether your jurisdiction considers that reportable abuse or permissible discipline.
Assess and Document Safety Concerns
When a teenager describes an older sibling’s inappropriate touching, you must recognize that as sexual abuse and understand your reporting window. When a family member expresses plans to harm themselves or another person, you must assess imminent danger versus general hopelessness and know whether your state’s duty to warn applies to family members or only to identifiable third parties.
Document your safety assessment with specificity that protects your license. Write down exactly what the person said, your clinical reasoning for whether it met the threshold for reporting, and what action you took. If you decided not to report, document why the behavior did not meet your state’s legal definition of reportable abuse or why the danger was not imminent. If you decided to report, document the date, time, agency you contacted, and the name of the person who received your report.
Handle Suicidal Ideation and Crisis Situations
Some therapists fear that documenting a decision not to report creates liability, but the opposite is true: failing to document your reasoning looks like you missed the problem entirely. The 988 Suicide and Crisis Lifeline provides immediate support when clients express suicidal ideation, and you should provide that number to every family or group participant at intake.
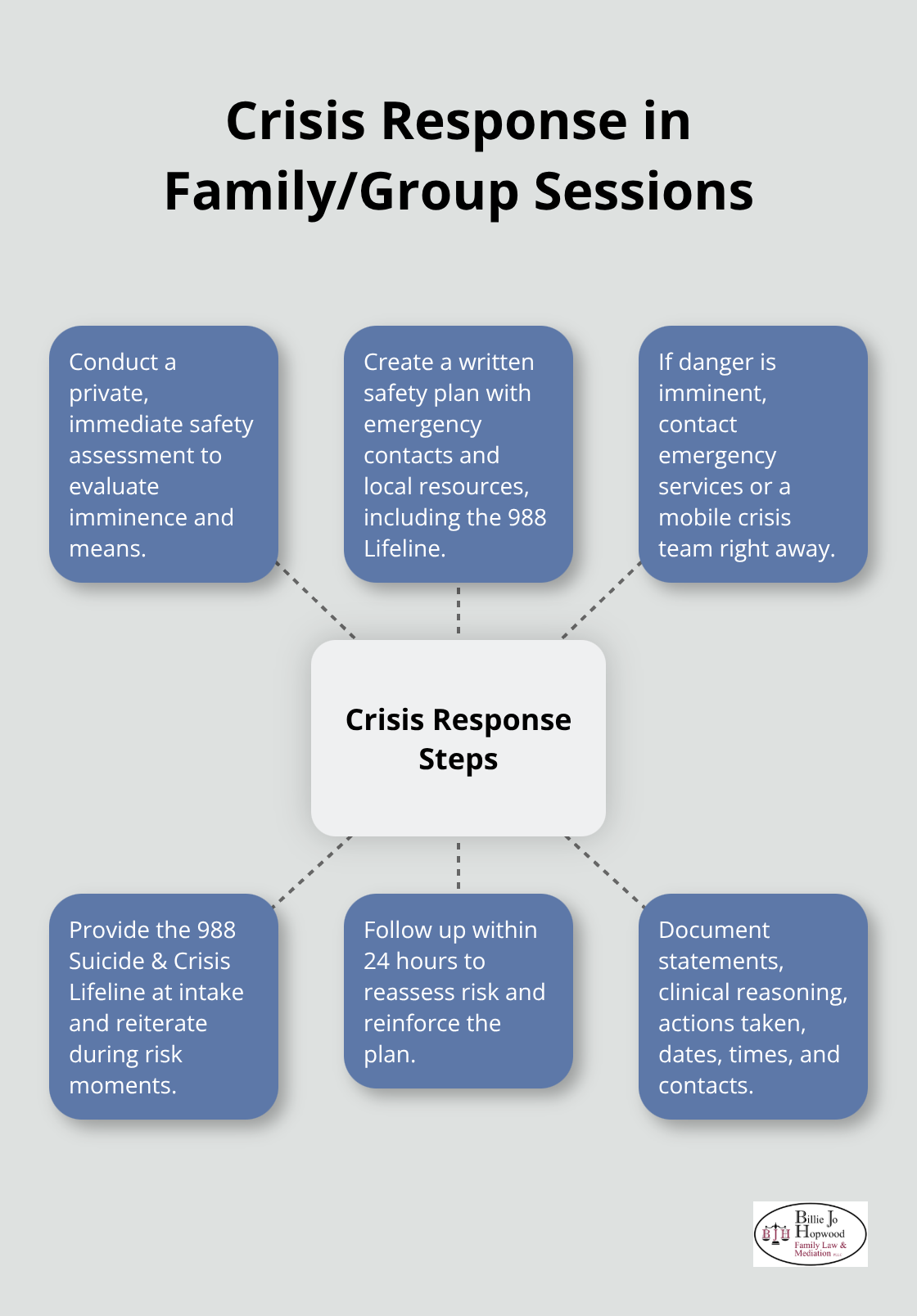
When someone in a family session says they have thought about killing themselves, do not rely on the family members present to keep them safe. Conduct a private safety assessment before the session ends, create a written safety plan with emergency contacts, and follow up within 24 hours. If imminent danger exists, contact emergency services or a crisis team directly.
Disclose Confidentiality Limits Upfront
Your written informed consent documents must clearly state that you will breach confidentiality to report abuse, prevent harm, or comply with court orders, and you must explain this at the first session without waiting for a crisis to arise. This transparency prevents clients from feeling blindsided when you must report, and it demonstrates your commitment to both legal compliance and ethical practice.
Final Thoughts
Documentation protects your practice and your clients simultaneously. Every confidentiality conversation, every safety assessment, every boundary intervention, and every decision to report or withhold information must appear in your clinical notes. Vague notes that say “discussed confidentiality” without specifics suggest you missed critical details, while detailed notes that explain what you said, how participants responded, and what you decided demonstrate you took your ethical duties seriously.
Transparent communication prevents most ethical problems before they start. Your written informed consent documents must address confidentiality limits, group rules, fees, cancellation policies, and what happens if someone breaches confidentiality. When you explain upfront that you will report abuse or imminent danger, clients understand your obligations rather than feeling betrayed when you must disclose information. Knowledge of your jurisdiction’s laws is non-negotiable-mandatory reporting thresholds, record retention requirements, and duty to warn standards vary by state, and Florida’s 24-hour reporting window for suspected child abuse differs from other states’ timelines.
If you work with families navigating divorce, custody disputes, or mediation, we at Billie Jo Hopwood Family Law & Mediation, PLLC in Melbourne, Florida understand the intersection of family law and therapeutic practice. When your clients need legal guidance alongside their therapeutic work, contact Billie Jo Hopwood Family Law & Mediation, PLLC for compassionate representation. Seek supervision regularly, especially when boundary questions or reporting decisions feel unclear, and stay informed about changes to professional codes as the legal and ethical landscape evolves.

